Welcome to our "Frequently Asked Questions" Page.
Can amplified pain be cured or it is just put in remission?
This is purely a matter of semantics. If all your symptoms go away and you are 100% fine, one could say you are cured. Our goal is cure. To say you are in remission gives the subtle and subconscious message that it is always lurking in the background. In the first study below, we documented that at 5 years after treatment 88% of children treated with exercise and counseling were fine. In the second study below 89% of the children fully resolved their symptoms. To say it is curative does not mean 100% of children with amplified pain will respond. This is true of everything in medicine. Not everyone with a staph infection is cured with antibiotics and if they are, they could always get staph again but we don’t say they are in remission. Likewise, some cancers can be removed or completely treated and are cured. You could say they are in remission but since it usually does not return, it is okay to say cured. Too often in medicine we are reluctant to use the word cure, but since many children with amplified pain resolve all symptoms for years, it is not unreasonable to say they are cured. There has also been stigma attached to the word cure with the FDA cracking down on peddlers of “cure-alls” and unscrupulous companies making false claims of curative products.
Adults, and children treated with drugs, generally only have temporary or incomplete benefit so historically physicians have not used the word cure.
Some of our patients have had relapses and that is always frustrating, but these children can respond well to re-treatment. Many of these children can retreat themselves without a full formal program. In the first study cited below, most who had a relapse were able to treat themselves and in the second study below, 5 of 7 children who had a relapse were able to treat themselves. In those who have relapsing amplified pain, there generally is a lot of underlying stress that needs to be addressed in addition to doing the exercise therapy.
- Sherry DD, Wallace CA, Kelley C, Kidder M, Sapp L. Short- and long-term outcomes of children with complex regional pain syndrome type I treated with exercise therapy. Clinical Journal of Pain 1999;15:218-23.
- Brooke V, Janselewitz S. Outcomes of children with complex regional pain syndrome after intensive inpatient rehabilitation. Pm & R 2012;4:349-54.
Can stomach problems be related to amplified pain?
Yes stomach problems can be directly related to amplified pain and we frequently see children with abdominal pain and dysfunction. Other possible causes of abdominal pain do need to be ruled out before a diagnosis of amplified pain of the abdomen can be made. It is important to make sure that children with stomach issues do not develop an eating disorder. It is imperative for these children to have a stable weight in order to participate in the intense physical and occupational therapy program.
Gastroparesis is a condition where there is delayed emptying of the stomach. The stomach and intestines are controlled by the autonomic, or automatic (fight or flight), nerves so it is not unusual for this to be part of amplified pain since it is through these nerves that the stomach symptoms become amplified. Along with these symptoms, stomach motility may be decreased. We treat it the same way as amplified pain, that is, with aerobic conditioning and desensitization. In children with gastroparesis we desensitize the stomach by putting food in the stomach frequently (breakfast, morning snack, lunch, afternoon snack, supper, evening snack, bedtime snack). The amount does not need to be large at first but it is important that they keep eating. We have had children who had zero motility on the repeated stomach emptying studies and, once they exercise and eat, their stomach motility has been documented to be above average. Medications for gastroparesis are fraught with side effects including causing stomach pain.
Irritable bowel syndrome can take on many different manifestations such as abdominal pain, gas, bloating, constipation mixed with diarrhea, and there may be motility issues such as gastroparesis (see above). The automatic, or autonomic nerves control the intestines, thus children who are prone to amplified pain, which is also controlled through the autonomic nerves, may also develop irritable bowel syndrome. In these children we emphasize continuing to be normally functioning regardless of symptoms. This means going to school, participating in aerobic training, and if there is pain with eating, to eat frequently, as we recommend for gastroparesis. If constipation is a significant problem then that needs to be treated specifically, just as any other medical condition needs to be treated. When these children are having frequent stools they still need to fully participate in life (school, shopping, visiting with friends) although they may need to have allowances for frequent trips to the bathroom. Once the diagnosis of irritable bowel syndrome has been made there should be no further testing done since there is the great temptation that just “one more test” well reveal a different diagnosis. Medications are generally not helpful for this. There has been a very good study of amitriptyline and children with irritable bowel syndrome that showed that it had no benefit over placebo.
_____________________________________________________________________________________________________________________________________
Amplified Abdominal Pain in Children
By Lori Brake, PTA; Jennifer Sherker, PsyD; David Sherry, MD; Kathy Fash, PT, DPT, CSCS, CBIS
Most commonly, children we see in our clinic will have Amplified Musculoskeletal Pain (AMP), also known as Complex Regional Pain Syndrome (CRPS), Reflex Sympathetic Dystrophy (RSD), Reflex Neurovascular Dystrophy (RND), or widespread pain such as in fibromyalgia. These conditions have historically been a challenging disorder for medical professionals to recognize and treat, and for patient and families who deal with prolonged pain and disability. Additionally patients and families may spend a prolonged time in the medical system before a correct diagnosis is arrived at and may undergo multiple therapeutic trials without success. Patients with autonomic features such as temperature changes, swelling, cyanosis, abnormal sweating, slow capillary refilling, atrophic skin changes, and allodynia (increased sensitivity to normal stimuli on skin) are more likely to be recognized earlier than those without such findings. Even so, many of the children we see have had months to even years of symptoms before diagnoses. In children with AMP, common treatment approaches include physical therapy, medications, nerve blocks, and surgical procedures; however, many medical interventions have various and limited outcomes often leading to only temporary resolution for children and adolescents who have been treated by those techniques. For examples, there is only a limited role for regional or sympathetic nerve blocks or narcotic analgesia in the management of Amplified Musculoskeletal Pain in children (Maillard, S., 2004).
The AMP program at The Children’s Hospital of Philadelphia uses a multidisciplinary exercise approach to treating AMP. This is a non-medication, function-based approach that concentrates on return to full function through an intensive exercise program and psychosocial support. Research shows that this approach helps children return to a full functional and, in most cases, a pain-free way of life (Sherry et al, 1991, 1992, 1999). Ultimately, it is the children who work through the pain and thus cure themselves.
While virtually any part of the body can be affected by pain, the focus of this article is on abdominal AMP. When amplified pain affects the patient’s abdomen and digestive tract, it often becomes even more challenging to obtain a correct diagnosis and treatment. For those who suffer from AMP of their abdomen, the symptoms can present themselves in a variety of ways including pain, nausea, difficulty eating or swallowing, and/or particular difficulties with specific food types. Although treatment approaches vary depending on what symptoms are present, the overall treatment approach is no different than treating amplified pain elsewhere in the body. It is important to focus on restoring function and strength through challenging those areas that are causing the most difficulty.
If abdominal AMP is suspected, it is important for the entire medical team to be on board together in making and understanding the diagnosis. Guidelines for identification of abdominal AMP type of pain have been published and can be used to guide the diagnostic process (Drossman, 2004). Once the diagnosis is made, it is important to discontinue further medical testing, pain medications (often, this is much harder on the doctors than on the patients) and make sure the patient, family and other medical providers understand AMP.
Our Treatment of Abdominal AMP
The overriding principle of our program is to have the children exercise and desensitize through the pain to establish normal function and eating. The amount of physical and occupational therapy varies tremendously between patients. Once children know that doing things that cause pain are not going to damage their body but actually help it heal, some will be able to establish normal function and resolve their pain on their own. However, for most children this hurts too much and they will need to work with a therapist. The amount of therapy can be as little as outpatient therapy several times a week to being hospitalized to receive up to 7 hours of physical and occupational therapy daily for many weeks. At The Children’s Hospital of Philadelphia children are treated as either Day Hospital patients (5 days a week from 8 AM to 4 PM) or as inpatients 7 days a week. Those with abdominal pain, especially because there are nutrition and eating issues, are generally best treated as inpatients at first so that appropriate monitoring can be done. Outlined below are some of the specific goals of our program.
Musculature: Core strengthening is an important part of any treatment program, but especially so when the pain is in the abdomen. Being creative with exercises is key to targeting those painful areas, thereby attacking the pain and leading to a more functional and hopefully less painful daily life. When first beginning to work on these exercises, many children are not accustomed to working those painful muscles and their body is often good at unconsciously or unwittingly compensating to avoid pain. Because of this, careful monitoring of position is important when exercising either by working out with someone who can help provide feedback or working in front of a mirror to self monitor position.
Examples of exercises that target abdominal pain: Push-ups, and holding push up position (planking) are very important exercise activities in treating abdominal pain. There are many ways in which this position can be incorporated into exercises, whether it is just holding the position, walking hands side to side while in this position, or even completing a puzzle or sorting shapes while holding a plank position. It is important for the body to be straight in order to ensure the abdominal muscles are fully engaged. If the patients’ hips are too bent, then the abdominal muscles do not have to work as hard, decreasing the effectiveness of the exercises. Walking up a steep hill out in the community or on a treadmill without holding onto the railings can be a great overall body workout and helps strengthen your abdominals and increase rotation. When doing exercises for the lower body, holding a ball out in front or overhead is an effective way to assist the abdominals in becoming engaged and this can be incorporated during squats, lunges, walking on knees, or moving from kneeling to standing repeatedly.
Pain to touch (allodynia): Incorporate desensitization into abdominal exercises whenever possible to help combat allodynia. With abdominal pain, the allodynia is often not just surface pain, but pressure pain when areas of the abdomen or ribs are pushed or massaged. What is used to desensitize varies from patient to patient and depends on what is most difficult and painful for each patient. For those who are sensitive to light touch, wearing fitted clothing may provide enough desensitization. For others, desensitization needs to be more rigorous. Plastic grass doormats from the local hardware store can be used to lie on or strapped to the stomach during exercises, tight shirts, tube tops with things like tennis balls, or Velcro tucked inside can also provide desensitization. The tennis balls are particularly helpful if the area is only sensitive to deep pressure. If touch is not an issue, but pressure is, then lying over a ball (playground, soccer, or basketball) while completing things such as a puzzle, or even while drawing, writing or coloring can be effective for desensitizing the area. Just like with the exercises, it is important to be creative with desensitization, and not always repeat the same strategies in order to keep motivation up and ensure the pain does not accommodate to just that one desensitization technique, but to all types of sensations.
Eating: Often when faced with AMP of the abdomen patients’ eating habits are affected. When eating is involved, it is always important to consider and evaluate the possibility of an underlying eating disorder; however eating disorders are not always present in patients with abdominal pain. The approach to this aspect of therapy is done under the guidance of the physician and where appropriate, nutritional specialist. If an eating disorder is suspected, it is important to refer the patient to the appropriate specialists. However, once an eating disorder has been ruled out and difficulties are primarily pain-related, snack time is typically incorporated during therapy sessions. Depending on how much else they are eating throughout the day, snack time may be as simple as eating a few crackers or may involve the intake of something more hearty and packed with calories and nutrients, such as nutritional shakes. The goals of this include both nutrition and desensitization. Additionally, eating at a normal speed is an issue for so many so eating may need to be timed and repeated if not at an age appropriate rate.
Stress: Stress can both cause and arise from abdominal pain. It is a classic symptom of children who first go to school and are suffering from the newness of a school situation and separation from their family. As mentioned above, children with amplified abdominal pain frequently have multiple diagnoses, procedures, medication without effect, suffer from isolation from peers, and many times professionals, teachers and friends do not believe they have as much pain as they have. This is very stressful and needs to be a part of a complete therapeutic program. We have a psychologist and music therapist help with coping strategies (sometimes co-treating in the gym), and allowing them to explore the meaning of the pain. School can be a major stress and our educator works with the child’s school to get them back into school with appropriate academic accommodation so that re-entry is as smooth as possible.
Outcomes
While research needs to be done to examine the effectiveness on this type of treatment for abdominal AMP, especially the physical and occupational therapy aspect, we do know that this approach has been very successful in resolving pain in the vast majority of patients treated for other types of amplified pain (Sherry, 1991, 1992, 1999) and we have had marked success in most of the children we see with abdominal pain. We, however, tend to see children who are significantly impaired due to their pain. Despite the pain, it does not have to interfere with function and is very treatable. Although the diagnostic and treatment process can be challenging, recognizing the symptoms, obtaining the appropriate diagnosis and engaging in treatment is key. It is important to be persistent and to educate patients, families, doctors, physical and occupational therapists and mental health professional that may be affected by this condition or treating someone who is. Treatment using a combination of exercise, desensitization, and eating, as well as psychosocial support can help patients increase and restore their function leading to decreased or resolved pain.
What can I do if I think I may be suffering from Abdominal AMP?
Talk with your medical professionals about your concerns and share information with them about AMP. Make sure you do not let the pain interfere with your life. Attend school and social events, and incorporate exercise into your daily routine, making sure to use those areas that are painful, including not only your abdominal muscles, but also your stomach itself. Additionally, carefully evaluate the role that stress in your life plays in your pain and the degree that the pain has caused you stress and have it evaluated by someone who has good insight into childhood psychological problems.
References
Camillieri M. “Management of patients with chronic abdominal pain in clinical practice.” Neurogastroenterology and motility. 2006;18:499-506.
Costanza CD, Longstreth GF, Liu AL. “Chronic abdominal wall pain: clinical features, health care costs, and long term outcomes.” Clinical Gastroenterology and Hepatology. 2004;2:395-399.
Drossman DA. “Functional abdominal pain syndrome.” Clinical Gastroenterology and Hepatology. 2004;2:353-365.
Maillard SM, et al. “Reflex Sympathetic Dystrophy: A Multidisciplinary Approach.”Arthritis Care and Research. 2004;51(2):284-290.
Rabinovich CE, Schanberg LE, Stein LD, Kredich DW. “ A Follow Up Study of Pediatric Fibromyalgia Patients” (abstract). Arthritis & Rheumatism.1990;33(suppl):S146.
Sherry DD, Wallace CA, Kelley C, Kidder M, Sapp L. “Short- and long-term outcomes of children with complex regional pain syndrome type I treated with exercise therapy.” Clinical Journal of Pain. 1999;15(3):218-223.
Sherry DD, McGuire T, Mellins E, Salmonsen K, Wallace CA, Nepom B. “Psychosomatic Musculoskeletal Pain in Childhood: clinical and psychological analyses of 100 children.” Pediatrics. 1991;88(6):1093-1099.
Sherry DD, Wallace CA. “Resolution of Fibromyalgia with an Intensive Exercise Program” (abstract). Clinical and Experimental Rheumatology. 1992;10:196.
Do you treat the pain or the dysfunction?
We do not treat the pain directly but focus on function. Most children, once function is restored, will lose their pain as a byproduct. There are children who will have long lasting pain and still have to live normal lives so will have to learn to cope with their pain in order to make it through the day and achieve their life goals. There are some treatment programs that expect all their patients to continue to have pain, so they focus on coping with pain, doing light activities, and life goal modification. While not achieved 100% of the time, total pain resolution should be the goal of every child with any form of amplified pain. We remain optimistic that a child will become fully functional and resolve all symptoms as this is what we experience in the majority of the cases we see. Even if they continue to have pain, virtually all the children who go through this program become fully functional unless they have prolonged conversion symptoms.
Children with amplified pain have varying degrees of physical dysfunction. Some are totally incapacitated and some are still going to school and participating in sports. Intense physical and occupational therapy programs address whatever deficits are at hand. If they cannot dress themselves, then dressing is the initial functional goal. If they cannot finish a soccer game, then we work more on strength and endurance. Every child is different and the program needs to be individually tailored to the child’s needs. Strength and endurance are common to all treatment programs. And in those with allodynia (tenderness to light touch) or other sensory pain, desensitization is also a significant portion of the program.
Does a patient have to go to a specialized treatment center?
The dose of exercise therapy varies from patient to patient. Some children can work through the pain on their own once they realize that they are not going to damage their body by using it. Other children can work well with a local physical therapist who will focus on function and desensitization as well as aerobic conditioning and not stop if the child complains of pain. In general, physical therapists are taught to stop when it hurts, which is excellent advice for everything except amplified pain. The amplified musculoskeletal pain team at the Children’s Hospital of Philadelphia is happy to assist your local health care professionals in gaining a better understanding of the principles of these amplified pain programs. More information can be found here.
Additionally, it is important to work with a psychologist to work on coping through the exercises and also address the individual and perhaps family dynamics to help relieve stress. Having pain is stressful in itself and prolonged amplified pain is emotionally distressing. The biochemical response to stress causes vasoconstriction, which can further exacerbate amplified pain symptoms. This is part of why it is very important to identify stressors and learn to better manage stress.
If the above is not effective, a larger dose of physical and occupational therapy with professionals who focus on treating amplified pain as well as working with mental health specialists who have extensive experience with this condition will be required. There is a list of programs in the United States here. A minority of children do not resolve their pain, even with this high dose of therapy.
Specialized programs to treat children with amplified pain have the added benefit of a community of children with whom they can relate. Many of these children feel isolated. Establishing a community to foster wellness can be a boon to both the patients and the team. Additionally, the experience of the specialized team can help determine when a child is ready to move on to the second stage of the program (home exercises, counseling, school, and full function).
Does this Treatment Program Work for Adults?
The best answer to this question is, unfortunately, that very little research has been done and we are not aware of any research done using this exact method.
We are aware of a study, done in the Netherlands, where 20 adults with complex regional pain syndrome (CRPS) did a progressive-loading exercise program with management of pain-avoidance behavior. Patients improved significantly with respect to pain and function. The authors conclude that it is a safe and effective method of treatment. The abstract can be found here.
As far as we are aware, there are no treatment programs designed for adults that offer the same level of intense physical and occupational therapy in conjunction with counseling. If you are aware of such a program or research for adults please let us know.
Children’s Specialized Hospital in New Brunswick does take patients up to age 21, though.
If you are a health care professional willing to treat adult AMPS patients who want this treatment, please let us know. The team at the Children’s Hospital of Philadelphia (CHOP) would be very interested in fostering an adult treatment program researching this intense exercise program. Please contact Dr. Sherry at the Children’s Hospital of Philadelphia AMPS Center (AMPSprogram@email.chop.edu) to express your interest in learning about and/or visiting the program.
Does weather affect the symptoms of amplified pain?
Many patients report feeling worse with changes in weather. However this seems to be very subjective and there are a couple of studies that have looked at this systematically and did not find a relationship between symptoms and temperature, barometric changes, humidity or season. We are not sure why people with amplified pain feel worse with changes in weather.
1. Bossema ER, van Middendorp H, Jacobs JW, Bijlsma JW, Geenen R. Influence of weather on daily symptoms of pain and fatigue in female patients with fibromyalgia: a multilevel regression analysis. Arthritis Care Res (Hoboken) 2013;65:1019-25.
2. Smedslund G, Eide H, Kristjansdottir OB, Nes AA, Sexton H, Fors EA. Do weather changes influence pain levels in women with fibromyalgia, and can psychosocial variables moderate these influences? International journal of biometeorology 2013.
I'm a health care professional. Can I get more information and support to help my AMPS patients?
Yes. The amplified musculoskeletal pain syndrome (AMPS) team at the Children’s Hospital of Philadelphia (University of Pennsylvania) welcomes physicians, physical and occupational therapists, mental health professionals, and other qualified health care providers to contact them at the AMPS center. The team can be reached at AMPSprogram@email.chop.edu.
If you have not seen the video, we recommend that you watch it as it may answer many questions. It gives in depth diagnostic and treatment guidelines for AMPS, including detailed PT/OT methods, a discussion on conversion, the psychological and school aspects of amplified pain, and seven patient stories of varying outcomes and forms of amplified pain.
If you are interested in starting an AMPS program at your facility (child or adult) you may be able to visit the AMPS program at the Children’s Hospital of Philadelphia or another AMPS program at one of the many hospitals in the US.
If you are simply looking for a program near you to send your patients to, please see our list of hospitals that offer this program.
Please also feel free to print and distribute the materials you find on this website. The AMPS Guide for Families, in particular, may be helpful to your patients.
Is amplified pain related to Lyme disease?
Lyme disease is an antibiotic sensitive infection. It is acquired through the bite of a deer tick. The tick needs to be attached at least 24 to 48 hours before it infects the host. The standard blood tests for Lyme disease are quite good. Initially, one does an ELISA screen and if that is positive, then Lyme disease is established by a positive Western blot test. The treatment is with antibiotics which are given for a duration of 2 to 4 weeks. There can be serious but rare complications of Lyme disease, some of which involve the heart or brain and require IV antibiotics. Anybody can get Lyme disease including children with amplified pain. Lyme may be the initial infection and after it is cured these children may have prolonged or remembered symptoms. We see patients who, after a sore throat, will have throat pain for weeks and the pain is worse than the original throat infection. The infection has cleared up but the symptoms remain and become amplified. Similarly, this can happen with Lyme, mononucleosis, injury or a host of other ills.
Some doctors propose there are patients with chronic Lyme who have tested negatively for Lyme. These physicians may use non-standardized tests such as urine tests to say that there is chronic Lyme disease. They propose long courses of IV or oral antibiotics. There is no evidence to support this. Good double-blind placebo-controlled trials have shown no benefit for long-term antibiotic use including no difference in cognitive function in those treated with antibiotics versus placebo.
1. Halperin JJ, Baker P, Wormser GP. Common misconceptions about Lyme disease. The American journal of medicine 2013;126:264.e1-7.
2. Klempner MS, Baker PJ, Shapiro ED, et al. Treatment trials for post-Lyme disease symptoms revisited. The American journal of medicine 2013;126:665-9.
3. Sigal LH, Patella SJ. Lyme arthritis as the incorrect diagnosis in pediatric and adolescent fibromyalgia. Pediatrics 1992;90:523-8.
4. Zotter S, Koch J, Schlachter K, et al. Neuropsychological profile of children after an episode of neuroborreliosis. Neuropediatrics 2013;44:346-53.
Is intense physical and occupational therapy without medications cruel?
At first it may seem cruel, but working through the pain not only saves the child from unnecessary risk and side effects of medications and procedures but also gives them the tools to stay well without needing to depend on health care professionals should they have a reoccurrence. Amplified pain is much more severe, but the principle is like when your leg falls asleep – it hurts to walk on it but the sooner you do the sooner it feels better. Amplified pain is cruel, not the treatment.
Kids like Matt (see Matt’s Story under patient videos here) had over 4 years of pain, failed multiple medications, had a pain pump surgically implanted and was still totally incapacitated. In 4 weeks of therapy, his pain resolved and he was able to have the pain pump removed. Another patient had 8 years of pain, including severe abdominal pain thought to be due to constipation to the point she had a colostomy. She had multiple IV medication trials and treatments. After 4 weeks of treatment her pain resolved, she was able to have her colostomy taken down, and spent her senior year going to school as any other normal teen after having missed most of high school.
Medications and procedures, in the children we feature in the video, do not work. To hold onto the hope of yet another pill or procedure is, in effect, more cruel than a few weeks of intense physical and occupational therapy. The children going through the program say that it is hard, but not cruel. It is trying, but there is a lot of emotional support for the children and their families. The health care professionals who work with these children are individuals who choose their career paths because they care about these kids. They are also cognizant of the child’s limits as they set attainable daily goals.
In quick summary, in a study of 70 children who were treated with drugs, only 42% resolved their symptoms, whereas in a study of 103 children treated with just an intense physical and occupational therapy program, 92% resolved all symptoms. Five years later 88% had no symptoms at the time of follow-up. In another study on intense physical and occupational therapy treatment, of 32 children, 89% resolved all their symptoms. These are the statistics that we have and we need to give these kids their best shot at beating amplified pain.
What hospitals offer this treatment program?
There are a number of treatment facilities that offer physical and occupational therapy programs for children with amplified musculoskeletal pain syndromes (AMPS) throughout the US, but we only include here hospital programs where the staff have trained directly with the Children’s Hospital of Philadelphia AMPS team and that we know have specifically modeled their programs after the program which produced the statistical data in the 1999 outcomes study, which demonstrates the effectiveness of this treatment (out of 103 patients, 92% had fully resolved their pain and 88% were pain free five years later).
We are not aware of any facilities that offer this type of program for adults. If you know of such a facility, please let us know via our contact page.
To get into an AMPS program you or your child first needs to be seen by a physician on a programs team, so the first step is to make a doctor’s appointment with the appropriate physician at the hospital you’re interested in. If you need help finding a physician, please send us an email though our contact form and we will do our best to help.
California
- San Diego – Rady Children’s Hospital, University of California, San Diego
- San Francisco – UCSF Benioff Children’s Hospital San Francisco, University of California, San Francisco
Massachusetts
- Boston – Boston Children’s Hospital: Pediatric Pain Rehabilitation Center, Harvard University
Missouri
- Kansas City – Children’s Mercy: Rehabilitation for Amplified Pain Syndrome (RAPS), University of Missouri
Nebraska
- Omaha – Children’s Hospital and Medical Center, University of Nebraska
- Children’s Hospital and Medical Center in Omaha NE has a modified day program designed to treat AMPS. It is a multidisciplinary treatment approach with specialties including Rehab, Behavioral Health, and Rheumatology. The program runs Mon-Fri with one hour of OT and one hour of PT from 8-10 am for 5 weeks total. It is integrated with behavioral health with both individual and group sessions once weekly.
- Wayne – Providence Medical Center
New Jersey
- New Brunswick – Children’s Specialized Hospital: Pain Management (they take patients up to 21 years of age)
Oregon
Pennsylvania
- Pittsburgh – The Hospital at The Children’s Institute: Pain Rehabilitation Program, University of Pittsburgh
- Philadelphia – The Children’s Hospital of Philadelphia: Amplified Musculoskeletal Pain Syndrome (AMPS) Program, University of Pennsylvania
What is Amplified Pain?
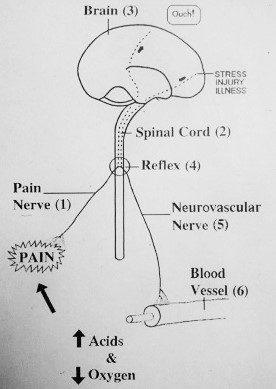
Amplified pain is pain that is out of proportion to the inciting stimulus. An example is when one has severe pain to just being lightly touched (allodynia) or to walking on a painful foot when there is no overt damage to the foot. The term amplified is used since a small sensory signal is amplified to the point it is unbearable. An analogy is when a microphone is placed too close to the speaker – you get very loud screeching feedback. The signal going into the microphone is soft but it comes out the speaker and goes back into the microphone and back out the speaker and thus sets up a vicious cycle resulting in a very loud sound. Even though the original hum coming from the speaker was soft, it becomes painfully loud.
In amplified pain, a very slight sensation can become unbearable pain as the nervous system sets up a feedback loop similar to the microphone example. The stimulus goes from the nerve to the spinal cord and then short-circuits to the autonomic nerves that control the blood vessels. This leads to lack of blood flow (ischemia) so the tissues do not get enough oxygen and there is a build-up of acids that lead to pain. This new pain signal is then again short-circuited to the autonomic nerves which again decrease the blood flow. This vicious cycle is how the pain is amplified (see image below). The pain is very real and this strong amplification is why medication typically does not work or only works temporarily.
The goal of the intense physical and occupational therapy used in pediatric Amplified Musculoskeletal Pain Syndrome (AMPS) programs at hospitals around the US, and shown in the video, is to retrain and desensitize the nervous system, breaking this pain cycle. This treatment method is successful in the vast majority of children and teens who have AMPS.
What is Pain?
As defined by the International Association for the Study of Pain, “Pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage.” Usually we think of pain when we get injured such as a cut or bruise. However, tissue damage in itself does not define pain; you can be shot in the leg and then run to save a friend and not know you have been shot even though there is a lot of tissue damage. You can also experience pain when you think you may have tissue damage such as having a sudden pang of pain when you put your hand on a stove burner until you realize that the stove is turned off. You can also have real chest pain when you have a broken heart (describing tissue damage) but your heart muscle itself is fine. Pain is always subjective; it is what the patient says it is.
What is postural orthostatic tachycardia syndrome (POTS) and is it related to amplified pain?
When you stand up suddenly there is a brief period of time that the blood flow to the brain is diminished and the heart rate increases to push more blood to the brain. It is common to feel a little dizzy when this happens. Children with POTS have an exaggerated response – they feel faint, dizzy and their heart rate increases at least 35 beats per minute over the rate when lying down (some authors say 45 beats in children). It typically affects adolescent girls and young women and tends to resolve with age. The standard treatment is to drink extra fluids and increase salt intake to increase the blood volume. Sometimes medications are used although recently it has been shown that doing cardiovascular conditioning exercises and core strengthening will reverse the symptoms. Some have argued that the manifestations of POTS are mostly due to deconditioning. We see children with amplified pain who have been diagnosed with POTS. The intense physical and occupational therapy program for amplified pain improves the POTS symptoms in these children.
POTS needs to be differentiated from conversion symptoms. Children can have conversion dizziness and other POTS-like conversion symptoms such as memory loss or cognitive difficulties.
1. Arnold AC, Okamoto LE, Diedrich A, et al. Low-dose propranolol and exercise capacity in postural tachycardia syndrome: a randomized study. Neurology 2013;80:1927-33.
2. Fu Q, Vangundy TB, Shibata S, Auchus RJ, Williams GH, Levine BD. Exercise training versus propranolol in the treatment of the postural orthostatic tachycardia syndrome. Hypertension 2011;58:167-75.
3. Joyner MJ. Exercise training in Postural Orthostatic Tachycardia syndrome: blocking the urge to block -receptors? Hypertension 2011;58:136-7.
4. Joyner MJ. Standing up for exercise: should deconditioning be medicalized? Journal of Physiology 2012;590:3413-4.
5. Singer W, Sletten DM, Opfer-Gehrking TL, Brands CK, Fischer PR, Low PA. Postural tachycardia in children and adolescents: what is abnormal? Journal of Pediatrics 2012;160:222-6.
6. Sukul D, Chelimsky TC, Chelimsky G. Pediatric autonomic testing: retrospective review of a large series. Clinical Pediatrics 2012;51:17-22.
Why are there so many different names for amplified musculoskeletal pain syndromes?
There are a lot of names for amplified pain since it can assume several forms and over time some doctors have divided amplified pain into different groups. Additionally, over time the name for the same condition has changed or some centers prefer their own name. It is somewhat like the proverbial blind men examining an elephant – some think the elephant is like a hose (the trunk), some like a wall (the side), some like a tree (the leg) and others like a snake (the tail).
Some children have very localized pain, that is, in just one part of their body. Some but not all of these children will have overt autonomic changes, that is, the hand or foot is cold, purple or blue and may be swollen and sweaty. If there are these autonomic changes present, the diagnosis is complex regional pain syndrome (CRPS) (which used to be called reflex sympathetic dystrophy (RSD)). If there are no autonomic changes it can be called localized amplified musculoskeletal pain, myofascial pain, neuropathic pain, or localized idiopathic pain.
If the pain is in three or more parts of the body, it can be called diffuse amplified musculoskeletal pain, diffuse idiopathic pain, myofascial pain syndrome, or neuropathic pain (among others) and some of these children with diffuse pain may fulfill criteria for juvenile fibromyalgia. Some doctors call these children total body RSD or total body CRPS but that is a misnomer. Additionally, there are children with intermittent forms or a combination of forms, one can have CRPS of the foot and total body pain, or fibromyalgia at the same time.
CRPS is the most obvious form because there are classic physical findings. Older terms for CRPS include reflex sympathetic dystrophy (RSD), shoulder hand syndrome, Suduck atrophy and allogodystrophy. Because it is so recognizable, many physicians do not see the relationship between CRPS and the other forms of amplified musculoskeletal pain. However, there is a significant overlap between CRPS and the other forms of amplified musculoskeletal pain since so many children have CRPS and either diffuse or localized amplified musculoskeletal pain as well. Also there are many children who have had CRPS who later develop a different form of amplified musculoskeletal pain.
The term RND has been used to refer to all children with amplified musculoskeletal pain or to children with CRPS since the mechanism for the amplification of pain is thought to be the same. Amplified musculoskeletal pain is now the preferred term and is used in the Textbook of Pediatric Rheumatology. RND was the term we used in 2002 and that is why you see it in the name of the foundation – “The Childhood RND Educational Foundation, Inc.”
It doesn’t matter what you call it, it all hurts severely and much more than one would typically suspect. The pain is very real. Regardless of the type of amplified pain they have, most children respond very well to the intensive treatment programs that are available at eight different hospitals in the US and detailed in our video.
Drugs and Other Treatments for Amplified Pain Syndromes:
There is a strong tendency to use medications or other procedures to try to treat the symptoms of the various forms of amplified pain. It is very hard for a physician facing a child in pain to not "do something." However, the evidence supporting the use of medications in children with amplified pain is slim to nonexistent and very real side effects can occur in patients when medications or procedures are used. Because the pain is amplified it is usually very resistant to traditional pain treatments or procedures. Sometimes there is an initial benefit but it generally wears off. Any evaluation of a treatment needs to include long-term results. There are too many treatments that have been touted as beneficial in a few patients but then, over the years, prove to be of no lasting or universal benefit.
The mind-body connection is significant in children with amplified pain and there is a propensity for these children to have a placebo effect. The very first child reported with complex regional pain syndrome (CRPS) spontaneously resolved all of her symptoms the day she was meant to see a psychologist and two days before she was scheduled for a nerve block. This is not to imply that the pain was “all in her head,” but that the sympathetic nerves causing the pain are intrinsically linked to our emotions. Therefore, expectations of benefit can play a major role in short-term studies. This is reflected in the fact that there are so many widely varying therapies that have been proposed as beneficial in amplified pain syndromes.
Our philosophy is that intense physical and occupational therapy done in conjunction with emotional support and counseling should be the first course of treatment for all children with amplified pain. It is very effective, it is supported by a large series of patients at multiple treatment centers, and it enables the child to address reoccurrences without medical intervention. Below are individual discussions on the evidence for drugs and interventions commonly used to treat amplified pain. Before embarking on any course of treatment, including intense physical and occupational therapy, the risks and benefits should be fully discussed with your health care providers.
Amitriptyline (Elavil®) or other Tricyclic Antidepressants
Amitriptyline is a tricyclic antidepressant medication and many physicians use it in low-dose in patients with amplified pain such as fibromyalgia. They speculate that it can help restore a more normal sleep pattern. However, studies specifically looking at whether or not it changes sleep (α-δ non-rapid eye movement sleep) show that it does not. An open label study of 175 adults with fibromyalgia showed that amitriptyline was equally effective as routine physical therapy over 6 months. In multicenter placebo-controlled trial of amitriptyline in 90 children with irritable bowel syndrome there was no difference between it and the placebo. A recent Cochrane systematic review of these medications in patients with fibromyalgia were disappointed that they found no supportive, unbiased evidence to substantiate its use. They conclude it will satisfactorily relieve pain in only a minority of patients.
Before starting amitriptyline, it is important that a cardiologist review an EKG on all patients to make sure there are no underlying heart problems. If these are present amitriptyline and tricyclic antidepressants can lead to serious heart problems.
Young people (up to age 24 years) taking amitriptyline are at an increased risk of suicide in the first few months and need to be monitored closely.
Other common side effects include:
- upset stomach
- drowsiness
- dizziness
- weakness
- insomnia
- weight gain
- headaches
- blurred vision
- photosensitivity
- dry mouth
- Carette S, Oakson G, Guimont C, Steriade M. Sleep electroencephalography and the clinical response to amitriptyline in patients with fibromyalgia. Arthritis & Rheumatism 1995;38:1211-7.
- Moore RA, Derry S, Aldington D, Cole P, Wiffen PJ. Amitriptyline for neuropathic pain and fibromyalgia in adults. Cochrane Database of Systematic Reviews 2012;12:CD008242.
- Joshi MN, Joshi R, Jain AP. Effect of amitriptyline vs. physiotherapy in management of fibromyalgia syndrome: What predicts a clinical benefit? Journal of Postgraduate Medicine 2009;55:185-9.
- Goldenberg D, Mayskiy M, Mossey C, Ruthazer R, Schmid C. A randomized, double-blind crossover trial of fluoxetine and amitriptyline in the treatment of fibromyalgia. Arthritis & Rheumatism 1996;39:1852-9.
- Saps M, Youssef N, Miranda A, et al. Multicenter, randomized, placebo-controlled trial of amitriptyline in children with functional gastrointestinal disorders. Gastroenterology 2009;137:1261-9.
- Patra KP, Sankararaman S, Jackson R, Hussain SZ. Significance of screening electrocardiogram before the initiation of amitriptyline therapy in children with functional abdominal pain. Clinical Pediatrics 2012;51:848-51.
Bisphosphonates: neridronate (Nerixia ®), pamidronate (Aredia ®), etc.
There are several reports of the usefulness of bisphosphonates in small groups of patients with complex regional pain syndrome (CRPS). Neridronate (which is not available in the United States at the time of this writing) was studied in 40 adults with CRPS in a double blinded placebo fashion (later 36 of the patients treated with placebo were treated with neridronate) and it was found to be beneficial for up to a year. Surprisingly, there is also good initial response in those treated with placebo. One limitation to this study was that they did not include patients who had had CRPS for longer than four months. A systematic review found strong evidence for the use of bisphosphonates in the short term but there been no long-term studies. There are some serious possible side effects including osteonecrosis of the jaw (death of the jaw bone) and optic neuritis and uveitis (inflammation of the eye).
One child with CRPS was given 11 treatments of pamidronate over two years along with physical therapy and did well. Further studies need to be done before this can be recommended, particularly in children. Bisphosphonates are in bones long-term, which raises concerns about long-term effects in children.
There are no studies of bisphosphonates in diffuse amplified pain syndromes, such as fibromyalgia.
Some possible side effects are:
- Muscle and joint pain
- Fever
- Tetany (low calcium levels)
- Osteonecrosis of the jaw (death of the jaw bone)
- Uveitis (inflammation of the eye)
- Cardiac arrhythmia
- Simm PJ, Briody J, McQuade M, Munns CF. The successful use of pamidronate in an 11-year-old girl with complex regional pain syndrome: response to treatment demonstrated by serial peripheral quantitative computerised tomographic scans. Bone 2010;46:885-8.
- Varenna M, Adami S, Rossini M, et al. Treatment of complex regional pain syndrome type I with neridronate: a randomized, double-blind, placebo-controlled study. Rheumatology 2013;52:534-42.
- Bittner T, Lorbeer N, Reuther T, et al. Hemimandibulectomy after bisphosphonate treatment for complex regional pain syndrome: a case report and review on the prevention and treatment of bisphosphonate-related osteonecrosis of the jaw. Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology 2012;113:41-7.
- Stack R, Tarr K. Drug-induced optic neuritis and uveitis secondary to bisphosphonates. New Zealand Medical Journal 2006;119:U1888.
Gabapentin (Neurontin®) or pregabalin (Lyrica®)
.
Gabapentin (Neurontin®) or pregabalin (Lyrica ®) are anti-epileptic drugs that are frequently used for neuropathic pain, such as prolonged pain after a case of shingles or nerve injury due to diabetes. There are also several other anti-epileptics, such as carbamazepine (Tegratol ®), that have been tried in chronic pain syndromes, but they are less frequently used. Lyrica ® is not presently approved for use in children.
A systematic review of both gabapentin and pregabalin in adult patients with fibromyalgia concluded that gabapentin was not very useful, but that pregabalin was likely effective. The caveat was that effectiveness was defined as only a 30% or more reduction in pain. Additionally, a quarter of patients had significant side effects requiring it to be stopped. A separate study showed that 1 out of 11 patients with fibromyalgia benefitted from pregabalin.
Young people (up to age 24 years) taking gabapentin or pregabalin are at an increased risk for suicide in the first few months and need to be monitored closely.
Common side effects include:
- Dizziness
- Drowsiness
- Dry mouth
- Weight gain
- Edema (swelling)
- Vision problems
- Muscle pain
- Behavioral changes (hostility, anxiety, panic attacks, depression)
- Tzellos TG, Toulis KA, Goulis DG, et al. Gabapentin and pregabalin in the treatment of fibromyalgia: a systematic review and a meta-analysis. Journal of Clinical Pharmacy & Therapeutics 2010;35:639-56.
- Wheeler DS, Vaux KK, Tam DA. Use of gabapentin in the treatment of childhood reflex sympathetic dystrophy. Pediatric Neurology 2000;22:220-1.
- Moore RA, Straube S, Wiffen PJ, Derry S, McQuay HJ. Pregabalin for acute and chronic pain in adults. Cochrane Database of Systematic Reviews 2009:CD007076.
- Roskell NS, Beard SM, Zhao Y, Le TK. A meta-analysis of pain response in the treatment of fibromyalgia. Pain Practice 2011;11:516-27.
Ketamine
Ketamine is an anesthetic agent related to PCP (angel dust). Because of this, it has the tendency to produce hallucinations and paranoid delusions. It has been studied in adults with CRPS and, over 12 weeks, there was a reduction in pain that was most notable the 1st week of therapy, but there was no difference between ketamine and placebo at the end of the study. Even with the reduction in pain, there was no improvement in function. In a study of oral ketamine in 12 children with chronic pain it seemed effective in 5, but did not last longer than 12 months and in the one child who had amplified musculoskeletal pain in this study, it was not helpful.
Ketamine comas are not approved in the United States, are very controversial, and have not been proven to have any lasting benefit. Ketamine comas have been associated with paralysis, pneumonia, and pulmonary embolus (which can be life-threatening).
There is increasing recognition of liver toxicity as well as prolonged mania.
We had one patient who, years later, was still suffering hallucinogenic flashbacks after having ketamine infusions. We saw another patient who did well initially after a ketamine coma in Germany, but after 40 booster ketamine injections she had such severe pain in her feet that she could not even touch them to the floor. Both of these patients did well in an intense physical and occupational therapy program.
Possible side effects of ketamine include:
- Death
- Hallucinations
- Prolonged Mania
- Paranoia
- Psychotic symptoms
- Liver toxicity
- Addiction/drug abuse
- Heart problems (arrhythmia)
- Breathing difficulties
- Ridged muscles
- Extreme pain
- Nausea and vomiting
- Sigtermans MJ, van Hilten JJ, Bauer MC, et al. Ketamine produces effective and long-term pain relief in patients with Complex Regional Pain Syndrome Type 1. Pain 2009;145:304-11.
- Patil S, Anitescu M. Efficacy of outpatient ketamine infusions in refractory chronic pain syndromes: a 5-year retrospective analysis. Pain Medicine 2012;13:263-9.
- Bredlau AL, McDermott MP, Adams HR, et al. Oral ketamine for children with chronic pain: a pilot phase 1 study. Journal of Pediatrics 2013;163:194-200.e1.
- Bell RF. Ketamine for chronic noncancer pain: concerns regarding toxicity. Current Opinion in Supportive & Palliative Care 2012;6:183-7.
- Noppers IM, Niesters M, Aarts LP, et al. Drug-induced liver injury following a repeated course of ketamine treatment for chronic pain in CRPS type 1 patients: a report of 3 cases. Pain 2011;152:2173-8.
- Ricke AK, Snook RJ, Anand A. Induction of prolonged mania during ketamine therapy for reflex sympathetic dystrophy. Biological Psychiatry 2011;70:e13-4.
- Sear JW. Ketamine hepato-toxicity in chronic pain management: another example of unexpected toxicity or a predicted result from previous clinical and pre-clinical data? Pain 2011;152:1946-7.
- Henson P, Bruehl S. Complex regional pain syndrome: state of the art update. Current treatment options in cardiovascular medicine 2010;12:156-67.
Spinal Cord Stimulators
Spinal cord stimulators apply a small electrical input via electrodes placed next to the spinal cord. They are surgically placed into the epidural space next to the spinal cord at a site that has been previously determined in a trial procedure to decrease pain. However, there is a high rate of movement of the electrodes, so they frequently migrate from the original place over the spinal cord. In complex regional pain syndrome (CRPS) they have been reported to transiently decrease the pain. They do not prevent the spread of CRPS. There have been no Cochrane systematic reviews of spinal cord stimulators in amplified pain syndromes, but there was one done pertaining to their use in cancer related pain that concluded there was insufficient evidence for the use of spinal cord stimulators in treating refractory cancer related pain. In one study, seven children with amplified pain had spinal cord stimulators implanted; two had no benefit, one had an infection and the rest experienced benefit. In another report, six children had only mild improvement or worsening of their pain with the spinal cord stimulator.
Because this is a surgical procedure, there are many side effects possible, including some that are quite serious. Reported side effects include spinal fluid leakage, urinary retention, conversion disorder, panic attacks, priapism (prolonged erections), infection, skin cancer and paralysis. One patient had permanent neurological damage when the spinal cord stimulator was uncontrollably activated by an antitheft device at a store.
It has been argued that since most children do well with conventional therapies (exercise therapy and counseling) invasive therapies should be avoided.
- Kumar K, Rizvi S, Bnurs SB. Spinal cord stimulation is effective in management of complex regional pain syndrome I: fact or fiction. Neurosurgery 2011;69:566-78; discussion 5578-80.
- Osborne MD, Ghazi SM, Palmer SC, Boone KM, Sletten CD, Nottmeier EW. Spinal cord stimulator–trial lead migration study. Pain Medicine 2011;12:204-8.
- Aldrete JA, Vascello LA, Ghaly R, Tomlin D. Paraplegia in a patient with an intrathecal catheter and a spinal cord stimulator. Anesthesiology 1994;81:1542-5; discussion 27A-28A.
- Arxer A, Busquets C, Vilaplana J, Villalonga A. Subacute epidural abscess after spinal cord stimulator implantation. European Journal of Anaesthesiology 2003;20:755-7.
- Falowski S, Ooi YC, Sabesan A, Sharan A. Spinal cord injury induced by a cervical spinal cord stimulator. Neuromodulation 2011;14:34-6; discussion 6-7.
- Gilbert JW, Wheeler GR, Mick GE, Herder SL, Richardson GB. Paraparesis following spinal cord stimulator trial, implantation and revision. Pain Physician 2010;13:E377.
- Han D, Connelly NR, Weintraub A, Kanev P, Solis E. Conversion locked-in syndrome after implantation of a spinal cord stimulator. Anesthesia & Analgesia 2007;104:163-5.
- Pope JE, Stanton-Hicks M. Accidental subdural spinal cord stimulator lead placement and stimulation. Neuromodulation 2011;14:30-2
- Zdanowicz N, Janne P, Reynaert C, Wunsch A. Induction of a schizophreniform disorder by a spinal cord stimulator. Psychosomatics 1999;40:76-8.
- Eisenberg E, Waisbrod H. Spinal cord stimulator activation by an antitheft device. Case report.[Erratum appears in J Neurosurg 1998 Apr;88(4):791]. Journal of Neurosurgery 1997;87:961-2.
- Olsson GL, Meyerson BA, Linderoth B. Spinal cord stimulation in adolescents with complex regional pain syndrome type I (CRPS-I). European Journal of Pain 2008;12:53-9.
- Wilder RT, Wilder RT. Management of pediatric patients with complex regional pain syndrome. Clinical Journal of Pain 2006;22:443-8.
- Lihua P, Su M, Zejun Z, Ke W, Bennett MI. Spinal cord stimulation for cancer-related pain in adults. The Cochrane database of systematic reviews 2013;2:Cd009389.Zernikow B, Dobe M, Hirschfeld G, Blankenburg M,
- Reuther M, Maier C. [Please don’t hurt me!: a plea against invasive procedures in children and adolescents with complex regional pain syndrome (CRPS)]. Der Schmerz 2012;26:389-95.
Steroids – prednisone, methylprednisolone (Medrol ®)
Steroids were used very early on in adults. In a small study they were found to be helpful. However, they had no appreciable effect in a small study of children with complex regional pain syndrome (CRPS). One investigator injected steroids intrathecally (into the spinal fluid), but the study was stopped due to side effects and lack of efficacy. Steroids have a host of significant side effects and are not recommended.
Side effects include (side effects increase with duration of treatment):
- Increased appetite
- Weight gain
- Suppressed immune system
- Osteoporosis
- Increased hair growth
- Acne
- Stretch marks
- Avascular necrosis of the bone
- High blood pressure
- Diabetes
- Growth retardation
- Psychosis
- Christensen K, Jensen EM, Noer I. The reflex dystrophy syndrome response to treatment with systemic corticosteroids. Acta Chirurgica Scandinavica 1982;148:653-5.
- Ruggeri SB, Athreya BH, Doughty R, Gregg JR, Das MM. Reflex sympathetic dystrophy in children. Clin Orthop Relat Res 1982; 163:225-30.
- Munts AG, van der Plas AA, Ferrari MD, Teepe-Twiss IM, Marinus J, van Hilten JJ. Efficacy and safety of a single intrathecal methylprednisolone bolus in chronic complex regional pain syndrome. European journal of pain (London, England) 2010;14:523-8.
Sympathectomy (cutting the sympathetic nerves)
Sympathectomy is done surgically, chemically or by radioablation. There is a recent Cochrane systematic review that concluded: “The practice of surgical and chemical sympathectomy for neuropathic pain and CRPS is based on very little high quality evidence. Sympathectomy should be used cautiously in clinical practice, in carefully selected patients, and probably only after failure of other treatment options. In these circumstances, establishing a clinical register of sympathectomy may help to inform treatment options on an individual patient basis.”
It has been argued that since most children do well with conventional therapies (exercise therapy and counseling) invasive therapies should be avoided.
- Straube S, Derry S, Moore RA, Cole P. Cervico-thoracic or lumbar sympathectomy for neuropathic pain and complex regional pain syndrome. Cochrane Database Syst Rev. 2013 Sep 2;9:CD002918. doi: 10.1002/14651858.CD002918.pub3.
- Zernikow B, Dobe M, Hirschfeld G, Blankenburg M, Reuther M, Maier C. [Please don’t hurt me!: a plea against invasive procedures in children and adolescents with complex regional pain syndrome (CRPS)]. Der Schmerz 2012;26:389-95.
Sympathetic blocks, nerve blocks and epidurals
It was thought that since amplified pain runs through the autonomic, or sympathetic nerves, that blocking or numbing these nerves would be beneficial. Typically, the reason given is to reduce pain to allow for more intense physical therapy. People have attempted this with guanethidine, reserpine, lumbar, axillary or stellate ganglion blocks. It was recognized early on that these do not have lasting effects and in 273 patients treated with sympathetic blockade only 7% had good or lasting results. A Cochrane systematic review was unable to determine if sympathetic blocks were effective and found little evidence to support them as standard of care in the treatment of CRPS. Sympathetic blocks for fibromyalgia have been done unsuccessfully. Sympathetic blocks have not been studied in children and have significant risks. One of my patients had her liver lacerated when they did a lumbar block and it had to be surgically repaired. Many prominent pediatric anesthesiologists no longer recommend sympathetic blocks in children.
There have been very few studies of peripheral blocks in children with CRPS and all have only reported extremely short term outcomes (most 2 months), but have reported benefit. Side effects, including seizures, have been reported.
In a study of 55 adults, Guanethidine blocks only helped 10% of the patients and 34% had significant side effects.
In lieu of blockade, some physicians will instill agents in the spinal fluid (epidural infusions). There have been no systematic studies of this in adults or children and there have been significant side effects reported including abscesses and sepsis in children.
It has been argued that since most children do well with conventional therapies (exercise therapy and counseling) invasive therapies should be avoided.
Possible side effects depend on the agent used and the location of the procedure.
- Veldman PH, Reynen HM, Arntz IE, Goris RJ. Signs and symptoms of reflex sympathetic dystrophy: prospective study of 829 patients. Lancet 1993;342:1012-6.
- Buchta RM. Reflex sympathetic dystrophy in a 14-year-old female. Journal of Adolescent Health Care 1983;4:121-2.
- Kaplan R, Claudio M, Kepes E, Gu XF. Intravenous guanethidine in patients with reflex sympathetic dystrophy. Acta Anaesthesiologica Scandinavica 1996;40:1216-22.
- Cepeda MS, Carr DB, Lau J. Local anesthetic sympathetic blockade for complex regional pain syndrome. Cochrane Database of Systematic Reviews 2005:CD004598.
- Dadure C, Motais F, Ricard C, Raux O, Troncin R, Capdevila X. Continuous peripheral nerve blocks at home for treatment of recurrent complex regional pain syndrome I in children. Anesthesiology 2005;102:387-91.
- Martin DP, Bhalla T, Rehman S, Tobias JD. Successive multisite peripheral nerve catheters for treatment of complex regional pain syndrome type I. Pediatrics 2013;131:e323-6.
- Bredahl C, Kristensen AK, Christensen KS, Bredahl C, Kristensen AK, Christensen KS. Treatment of reflex dystrophy with continuous peripheral nerve block. Ugeskrift for Laeger 2007;169:59-60.
- Ahmed SU, Vallejo R, Hord ED. Seizures after a Bier block with clonidine and lidocaine. Anesthesia & Analgesia 2004;99:593-4
- Lundborg C, Dahm P, Nitescu P, Appelgren L, Curelaru I. Clinical experience using intrathecal (IT) bupivacaine infusion in three patients with complex regional pain syndrome type I (CRPS-I). Acta Anaesthesiologica Scandinavica 1999;43:667-78.
- Ingelmo PM, Marino G, Fumagalli R. Sepsis after epidural catheterization in a child with chronic regional pain syndrome type I. Paediatric Anaesthesia 2005;15:623-4.
- Lin YC, Greco C. Epidural abscess following epidural analgesia in pediatric patients. Paediatric Anaesthesia 2005;15:767-70.
- Wilder RT. Management of pediatric patients with complex regional pain syndrome. Clinical Journal of Pain 2006;22:443-8.
- Zernikow B, Dobe M, Hirschfeld G, Blankenburg M, Reuther M, Maier C. [Please don’t hurt me!: a plea against invasive procedures in children and adolescents with complex regional pain syndrome (CRPS)]. Der Schmerz 2012;26:389-95.
Patient Videos

Matt's story
Diffuse Amplified Pain (Myofascial Pain, Fibromyalgia, etc.)

ALISSA'S STORY
Localized Amplified Pain (CRPS, RSD, etc.)
